RESEARCH PAPER
Various forms of heat therapy and the quality of life of women with dysmenorrhea. A preliminary study
1
Faculty of Health Sciences, Medical University of Gdańsk, Gdańsk, Poland
2
Department of Radiological Informatics and Statistics, Medical University of Gdańsk, Gdańsk, Poland
3
Department of Rehabilitation Medicine, Medical University of Gdańsk, Gdańsk, Poland
4
Department of Gynecology, Obstetrics and Neonatology, Medical University of Gdańsk, Gdańsk, Poland
5
Department of Immunobiology and Environment Microbiology, Medical University of Gdańsk, Gdańsk, Poland
Corresponding author
Katarzyna Zorena
Department of Immunobiology and Environment Microbiology, Medical University of Gdańsk, Gdańsk, Polska
Department of Immunobiology and Environment Microbiology, Medical University of Gdańsk, Gdańsk, Polska
Med Srod. 2024;27(2):95-101
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
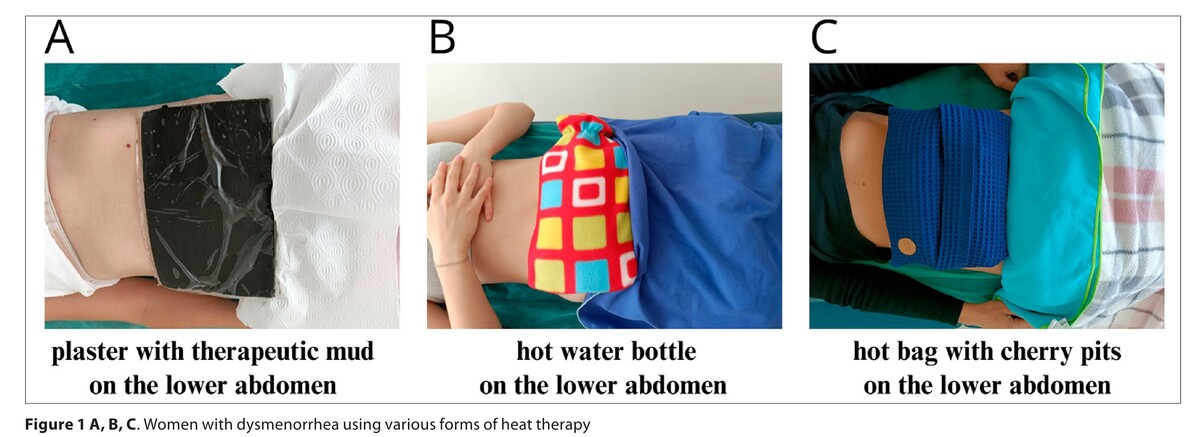
The aim of the study was to assess the impact of heat therapy using plaster with therapeutic mud, hot water bottle and hot bag with cherry pits on the quality of life of young women with dysmenorrhea.
Material and methods:
Thirty women with dysmenorrhea aged 18–34 (median: 22.50 years, first quartile: 21.00 years, and third quartile: 23.75 years) were randomly assigned to three groups: group 1 – used a plaster with therapeutic mud, group 2 – hot water bottle, and group 3 – a hot bag with cherry pits. Basic data was collected using a questionnaire. Therapy started 3–5 days before menstruation, warm compress was applied three times (once a day) for 20 minutes in the lower abdomen or lumbar region, depending on where women experienced more pain during menstruation. Using a Visual Analogue Scale (VAS) to assess pain level and the Likert scale to assess quality of life, menstruation after heat therapy was compared with previous cycles.
Results:
Women with dysmenorrhea experienced changes in the perception of lower abdominal and lumbar pain post-heat therapy. Based on VAS, a significantly lower level of lumbar pain was observed post mud therapy vs. pre-therapy (p-value=0.013). A significantly lower level of lower abdominal pain post vs. pre-therapy using a hot bag with cherry pits was reported (p-value=0.006). Moreover, 46.7% of women were satisfied with the therapy, and 93.3% would like to continue heat therapy in the following months. Quality of life according to the Likert scale improved in 9 women in Group 1, 8 women in Group 2 and 7 women in Group 3. However, no statistical significance between groups was demonstrated (p-value=0.877).
Conclusions:
According to the preliminary results, heat therapy applied a few days before menstruation can reduce dysmenorrhea and may be a good addition to pharmacological treatment.
The aim of the study was to assess the impact of heat therapy using plaster with therapeutic mud, hot water bottle and hot bag with cherry pits on the quality of life of young women with dysmenorrhea.
Material and methods:
Thirty women with dysmenorrhea aged 18–34 (median: 22.50 years, first quartile: 21.00 years, and third quartile: 23.75 years) were randomly assigned to three groups: group 1 – used a plaster with therapeutic mud, group 2 – hot water bottle, and group 3 – a hot bag with cherry pits. Basic data was collected using a questionnaire. Therapy started 3–5 days before menstruation, warm compress was applied three times (once a day) for 20 minutes in the lower abdomen or lumbar region, depending on where women experienced more pain during menstruation. Using a Visual Analogue Scale (VAS) to assess pain level and the Likert scale to assess quality of life, menstruation after heat therapy was compared with previous cycles.
Results:
Women with dysmenorrhea experienced changes in the perception of lower abdominal and lumbar pain post-heat therapy. Based on VAS, a significantly lower level of lumbar pain was observed post mud therapy vs. pre-therapy (p-value=0.013). A significantly lower level of lower abdominal pain post vs. pre-therapy using a hot bag with cherry pits was reported (p-value=0.006). Moreover, 46.7% of women were satisfied with the therapy, and 93.3% would like to continue heat therapy in the following months. Quality of life according to the Likert scale improved in 9 women in Group 1, 8 women in Group 2 and 7 women in Group 3. However, no statistical significance between groups was demonstrated (p-value=0.877).
Conclusions:
According to the preliminary results, heat therapy applied a few days before menstruation can reduce dysmenorrhea and may be a good addition to pharmacological treatment.
REFERENCES (24)
1.
Nyirenda T, Nyagumbo E, Murewanhema G, et al. Prevalence of dysmenorrhea and associated risk factors among university students in Zimbabwe. Womens Health (Lond). 2023;19. https://doi.org/10.1177/174550....
2.
Barcikowska Z, Wójcik-Bilkiewicz K, Sobierajska-Rek A, et al. Dysmenorrhea and Associated Factors among Polish Women: A Cross Sectional Study. Pain Res Manag. 2020. https://doi.org/10.1155/2020/6....
3.
Guimarães I, Póvoa AM. Primary Dysmenorrhea: Assessment and Treatment. Rev Bras Ginecol Obstet. 2020;42(8):501–507. https://doi.org/10.1055/s-0040....
4.
Sachedina A, Todd N. Dysmenorrhea, Endometriosis and Chronic Pelvic Pain in Adolescents. J Clin Res Pediatr Endocrinol. 2020;12(Suppl 1):7–17. https://doi.org/10.4274/jcrpe.....
5.
Armour M, Smith CA, Steel KA, et al. The effectiveness of self-care and lifestyle interventions in primary dysmenorrhea: a systematic review and meta-analysis. BMC Complement Altern Med. 2019;19(1):22. https://doi.org/10.1186/s12906....
6.
Nie W, Xu P, Hao C, et al. Efficacy and safety of over-the-counter analgesics for primary dysmenorrhea: A network meta-analysis. Medicine (Baltimore). 2020;99(19). https://doi.org/10.1097/MD.000....
7.
Kirca N, Celik AS. The effect of yoga on pain level in primary dysmenorrhea. Health Care Women Int. 2023;44(5):601–620. https://doi.org/10.1080/073993....
8.
Armour M, Ee CC, Naidoo D, et al. Exercise for dysmenorrhoea. Cochrane Database Syst Rev. 2019; 9(9). https://doi.org/10.1002/146518....
9.
Trybulec B, Wyżycka E. The use of selected techniques of manual therapy in conservative treatment of primary dysmenorrhea. Med Rev. 2016;14(2):162–172. https://doi.org/10.15584/medre....
10.
Saputri FR, Ardana SDS, Ayuningtias DR, et al. The Effectiveness of Warm Compress Against Primary Dysmenorrhea Pain. Prosiding University Research Colloquium. 2022;128–133.
11.
Budiarti R, Yulianti L. The Effect of Warm Compresses on Reducing Dysmenorrhea Pain in Women of Childbearing Age at the Bungursari Health Center, Purwakarta Regency, Indonesia. AMCR. 2023;4(3):437–440. https://doi.org/10.37275/amcr.....
12.
Safitri M, Dwi Jayanti R, Erye Frety E. Comparison of the effectiveness of giving warm compresses and cold compresses in handling dysmenorrhea: Systematic review. World J Adv Res Rev. 2023;18(3):585–590. https://doi.org/10.30574/wjarr....
13.
Mukhoirotin K, Fatmawati D. The Effectivity of Cold Compress and Warm Compress to Intensity Level of Menstrual Pain (Dysmenorrhea). The 4th International Conference on Nursing, 2018.
14.
Chaudhuri A, Singh A, Dhaliwal L. A randomised controlled trial of exercise and hot water bottle in the management of dysmenorrhoea in school girls of Chandigarh, India. Indian J Physiol Pharmacol. 2013;57(2):114–122.
15.
Vilšinskaitė DS, Vaidokaitė G, Mačys Ž, et al. The risk factors of dysmenorrhea in young women. Wiad Lek. 2019;72(6):1170–1174.
16.
Delgado DA, Lambert BS, Boutris N, et al. Validation of Digital Visual Analog Scale Pain Scoring With a Traditional Paper-based Visual Analog Scale in Adults. J Am Acad Orthop Surg Glob Res Rev. 2018;2(3). https://doi.org/10.5435/JAAOSG....
17.
Tullis T, Bill A. Measuring the User Experience. 2nd ed. San Francisco, CA, USA: Morgan Kaufmann Publishers Inc.; 2013.
18.
R Core Team (2021). R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. URL https://www.R project.org/.
19.
Wang L, Yan Y, Qiu H, et al. Prevalence and Risk Factors of Primary Dysmenorrhea in Students: A Meta-Analysis. Value Health. 2022;25:1678–1684. https://doi.org/ 10.1016/j.jval.2022.03.023.
20.
Strocen E, Kawa M, Podgórska M. Skuteczność okładów borowinowych i sonoterapii w obniżeniu objawów choroby zwyrodnieniowej stawu kolanowego. Rocznik Naukowy. 2017;44–55.
21.
Demirel G, Çakir F. Heat, Cold Applications and Women's Health. Advances in Health Sciences Research. 2020; 243.
22.
Mori MM, Busoli Badiale S, Pastoris O, et al. Clinical monitoring of safety and functionality of a non-medicated patch for pain alleviation associated to dysmenorrhea. Acta Biomed. 2019;90(3):287–292. https://doi.org/10.23750/abm.v....
23.
Barcikowska Z, Rajkowska-Labon E, Grzybowska ME, et al. An Evaluation of the Effectiveness of Ibuprofen and Manual Therapy in Young Women with Dysmenorrhea-A Pilot Study. Healthcare (Basel). 2021;9(6):617. https://doi.org/10.3390/health....
24.
Barcikowska Z, Grzybowska ME, Wąż P, et al. Effect of Manual Therapy Compared to Ibuprofen on Primary Dysmenorrhea in Young Women-Concentration Assessment of C-Reactive Protein, Vascular Endothelial Growth Factor, Prostaglandins and Sex Hormones. J Clin Med. 2022;11(10):2686. https://doi.org/doi:10.3390/jc....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.