Online first
Bieżący numer
O czasopiśmie
Archiwum
Polityka etyki publikacyjnej
System antyplagiatowy
Instrukcje dla Autorów
Instrukcje dla Recenzentów
Rada Redakcyjna
Bazy indeksacyjne
Komitet Redakcyjny
Recenzenci
2024
2023
2022
2021
2020
2019
2018
Kontakt
Klauzula przetwarzania danych osobowych (RODO)
PRACA POGLĄDOWA
Ekspozom jamy ustnej: uwarunkowania środowiskowe w etiologii schorzeń jamy ustnej
1
Stażysta, Niepubliczny Zakład Opieki Zdrowotnej Mix-Med Arima
2
Internship, Wojskowy Instytut Medyczny - Państwowy Instytut Badawczy
3
Internship, Samodzielny Publiczny Zakład Opieki Zdrowotnej Wojewódzki Szpital Zespolony im. Jędrzeja Śniadeckiego w Białymstoku
4
Stażysta, Uniwersytecki Szpital Kliniczny nr 1 w Lublinie
Autor do korespondencji
Med Srod. 2026;29(1):14-19
SŁOWA KLUCZOWE
DZIEDZINY
STRESZCZENIE
Wprowadzenie i cel:
Choroby jamy ustnej pozostają istotnym globalnym wyzwaniem zdrowotnym, dotykając około 3,5 mld ludzi. Gdy tradycyjne modele etiologiczne skupiały się głównie na czynnikach behawioralnych i mikrobiologicznych, nieproporcjonalne obciążenie chorobami w regionach uprzemysławiających się sugeruje obecność przeoczonych determinantów niebehawioralnych. Niniejszy przegląd ma na celu syntezę obecnej literatury na temat ekspozomu jamy ustnej, a także przedstawienie analizy, w jaki sposób determinanty środowiskowe (zanieczyszczenia atmosferyczne, metale ciężkie i zanieczyszczenia chemiczne) wpływają na zdrowie jamy ustnej w ciągu życia.
Opis stanu wiedzy:
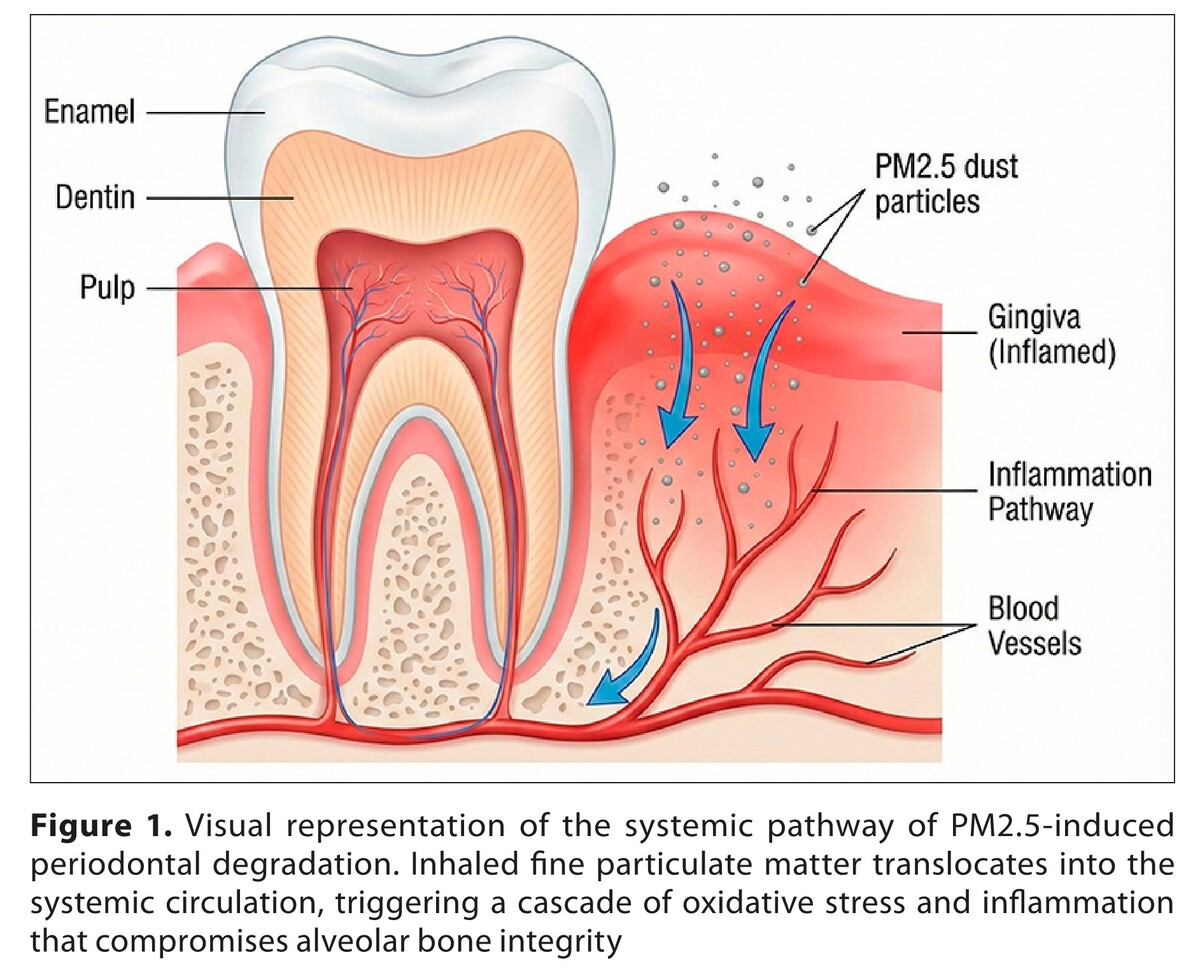
Badania sugerują, że toksyny środowiskowe działają jak stresory, zaburzając homeostazę jamy ustnej. W próchnicy narażenie na bierne palenie (SHS) osłabia odporność, a metale ciężkie (np. ołów) wywołują hipoplazję szkliwa poprzez substytucję jonową. Drobny pył i kadm wpływają na przyzębie, wyzwalając stres oksydacyjny i zapalenie, co przyspiesza resorpcję kości. Ponadto narażenie kobiety w ciąży na zanieczyszczenie powietrza atmosferycznego i zagrożenia zawodowe działa jako krytyczny teratogen powodujący rozszczepy ustno-twarzowe płodu. Badania wiążą też zanieczyszczenia gazowe i formaldehyd z rakiem nosogardła.
Podsumowanie:
Dowody wskazują na konieczność włączenia oceny ryzyka środowiskowego do profilaktyki stomatologicznej. Zanieczyszczenia są mimowolnymi czynnikami ryzyka działającymi synergistycznie z innymi determinantami. W celu zmniejszenia obciążenia chorobami i kształtowania polityki zdrowotnej niezbędne są strategie łagodzące skutki tych zjawisk.
Choroby jamy ustnej pozostają istotnym globalnym wyzwaniem zdrowotnym, dotykając około 3,5 mld ludzi. Gdy tradycyjne modele etiologiczne skupiały się głównie na czynnikach behawioralnych i mikrobiologicznych, nieproporcjonalne obciążenie chorobami w regionach uprzemysławiających się sugeruje obecność przeoczonych determinantów niebehawioralnych. Niniejszy przegląd ma na celu syntezę obecnej literatury na temat ekspozomu jamy ustnej, a także przedstawienie analizy, w jaki sposób determinanty środowiskowe (zanieczyszczenia atmosferyczne, metale ciężkie i zanieczyszczenia chemiczne) wpływają na zdrowie jamy ustnej w ciągu życia.
Opis stanu wiedzy:
Badania sugerują, że toksyny środowiskowe działają jak stresory, zaburzając homeostazę jamy ustnej. W próchnicy narażenie na bierne palenie (SHS) osłabia odporność, a metale ciężkie (np. ołów) wywołują hipoplazję szkliwa poprzez substytucję jonową. Drobny pył i kadm wpływają na przyzębie, wyzwalając stres oksydacyjny i zapalenie, co przyspiesza resorpcję kości. Ponadto narażenie kobiety w ciąży na zanieczyszczenie powietrza atmosferycznego i zagrożenia zawodowe działa jako krytyczny teratogen powodujący rozszczepy ustno-twarzowe płodu. Badania wiążą też zanieczyszczenia gazowe i formaldehyd z rakiem nosogardła.
Podsumowanie:
Dowody wskazują na konieczność włączenia oceny ryzyka środowiskowego do profilaktyki stomatologicznej. Zanieczyszczenia są mimowolnymi czynnikami ryzyka działającymi synergistycznie z innymi determinantami. W celu zmniejszenia obciążenia chorobami i kształtowania polityki zdrowotnej niezbędne są strategie łagodzące skutki tych zjawisk.
Introduction:
Oral diseases remain a major global health challenge, affecting app. 3.5 billion people. While traditional etiological models have focused primarily on behavioural and microbial factors, the disproportionate disease burden in industrializing regions suggests the presence of overlooked non-behavioural determinants.
Objective:
The aim of the review is to synthesize current literature regarding the ‘oral exposome’ analyzing how environmental determinants-specifically atmospheric pollutants, heavy metals and chemical contaminants impact oral health throughout the lifespan.
Brief description of the state of knowledge:
Recent research suggests that environmental toxicants may act as systemic stressors, potentially compromising oral homeostasis through a variety of mechanisms. Regarding dental caries, exposure to second-hand smoke (SHS) suppresses local immune responses, while heavy metals, such as lead, induce enamel hypoplasia via ionic substitution in the hydroxyapatite lattice. Periodontal health is similarly modulated by environmental factors, fine particulate matter and cadmium exposure trigger systemic oxidative stress and inflammation, accelerating alveolar bone resorption. Furthermore, maternal exposure to ambient air pollution and occupational hazards acts as a critical teratogen for orofacial clefts, particularly when interacting with genetic variants in folate metabolism. Finally, longitudinal data implicate gaseous pollutants and formaldehyde in the pathogenesis of nasopharyngeal carcinoma.
Summary:
Evidence necessitates integrating environmental risk assessment into preventive dentistry. Pollutants are involuntary risk factors acting synergistically with other determinants. Mitigation strategies are urgent for reducing the disease burden and informing policy.
Oral diseases remain a major global health challenge, affecting app. 3.5 billion people. While traditional etiological models have focused primarily on behavioural and microbial factors, the disproportionate disease burden in industrializing regions suggests the presence of overlooked non-behavioural determinants.
Objective:
The aim of the review is to synthesize current literature regarding the ‘oral exposome’ analyzing how environmental determinants-specifically atmospheric pollutants, heavy metals and chemical contaminants impact oral health throughout the lifespan.
Brief description of the state of knowledge:
Recent research suggests that environmental toxicants may act as systemic stressors, potentially compromising oral homeostasis through a variety of mechanisms. Regarding dental caries, exposure to second-hand smoke (SHS) suppresses local immune responses, while heavy metals, such as lead, induce enamel hypoplasia via ionic substitution in the hydroxyapatite lattice. Periodontal health is similarly modulated by environmental factors, fine particulate matter and cadmium exposure trigger systemic oxidative stress and inflammation, accelerating alveolar bone resorption. Furthermore, maternal exposure to ambient air pollution and occupational hazards acts as a critical teratogen for orofacial clefts, particularly when interacting with genetic variants in folate metabolism. Finally, longitudinal data implicate gaseous pollutants and formaldehyde in the pathogenesis of nasopharyngeal carcinoma.
Summary:
Evidence necessitates integrating environmental risk assessment into preventive dentistry. Pollutants are involuntary risk factors acting synergistically with other determinants. Mitigation strategies are urgent for reducing the disease burden and informing policy.
REFERENCJE (35)
1.
World Health Organization. Global oral health status report: towards universal health coverage for oral health by 2030. Geneva: World Health Organization; 2022. https://www.who.int/publicatio....
2.
Peres MA, Macpherson LM, Weyant RJ, et al. Oral diseases: a global public health challenge. Lancet. 2019;394(10194):249–260. https://doi.org/10.1016/S0140-....
3.
Landrigan PJ, Fuller R, Acosta NJ, et al. The Lancet Commission on pollution and health. Lancet. 2018;391(10119):462–512. https://doi.org/10.1016/S0140-....
4.
Chang ET, Ye W, Zeng YX, et al. The Evolving Epidemiology of Nasopharyngeal Carcinoma. Cancer Epidemiol Biomarkers Prev. 2021;30(6):1035–1047. https://doi.org/10.1158/1055-9....
5.
Wild CP, Place N. The exposome: a new concept for public health surveillance. Int J Epidemiol. 2017;46(2):415–427. https://doi.org/10.1093/ije/dy....
6.
Mehta AJ, Thalib L. A systematic review of the association between air pollution and periodontitis. Int J Environ Res Public Health. 2016;13(10):966. https://doi.org/10.3390/ijerph....
7.
Arora M, Austin C. Environmental exposures and developmental dental defects: A review of the evidence. Curr Oral Health Rep. 2015;2(1):15–22. https://doi.org/10.1007/s40496....
8.
Zhou Q, Zhang S, Wang Z, et al. Ambient air pollution and risk of non-syndromic orofacial clefts: A systematic review and meta-analysis. Environ Pollut. 2020;260:114002. https://doi.org/10.1016/j.envp....
9.
Huang H, Yan Y, Chiang C, et al. Association between secondhand smoke and dental caries in children and adolescents: A meta-analysis. Tob Induc Dis. 2020;18:78. https://doi.org/10.18332/tid/1....
10.
Deng X, Li Y, Sun X. Association between maternal smoking during pregnancy and dental caries in children: A systematic review and meta-analysis. Front Public Health. 2024;12:1339012. https://doi.org/10.3389/fpubh.....
11.
Wiener RC, Vatsky SR. Blood Lead Levels and Dental Caries in Children: An Analysis of NHANES 2015–2016. J Public Health Dent. 2021;81(1):58–64. https://doi.org/10.1111/jphd.1....
12.
Masarwa R, Levine H, Ginsberg G, et al. Association between exposure to bisphenol A and dental caries: a systematic review and meta-analysis. Environ Sci Pollut Res Int. 2020;27:16033–16041. https://doi.org/10.1007/s11356....
13.
Alkhobaizi Q, Al-Sane M, Seneviratne CJ. The Association between Bisphenol A and Dental Caries: A Systematic Review. Children (Basel). 2022;9(5):674. https://doi.org/10.3390/childr....
14.
Ljubicic M, Hauge A, Stenfors N. The association between air pollution and oral health in children and adolescents: A systematic review. Int J Environ Res Public Health. 2022;19(23):16220. https://doi.org/10.3390/ijerph....
15.
Shao J, Wu L, Leng WD. Association between exposure to environmental tobacco smoke and periodontal disease: A systematic review and meta-analysis. Front Public Health. 2023;11:1096645. https://doi.org/10.3389/fpubh.....
16.
Alanazi H, Semlali A, Chmielewski W, et al. Cytotoxic and pro-inflammatory effects of electronic cigarette fluids on human periodontal ligament fibroblasts. J Oral Sci. 2022;64(2):163–169. https://doi.org/10.2334/josnus....
17.
Deng S, Hu J, Zhang Y. Association between air pollution and periodontitis: A systematic review and meta-analysis. Environ Sci Pollut Res Int. 2023;30(12):32145–32158. https://doi.org/10.1007/s11356....
18.
Liao Y, Li D, Zhang Y. Association between blood cadmium levels and periodontitis: Evidence from NHANES 2013–2018. Front Public Health. 2023;11:1134582. https://doi.org/10.3389/fpubh.....
19.
Radke EG, Galizia A, Thayer KA, et al. Phthalate exposure and metabolic effects: a systematic review of the human epidemiological evidence. Environ Int. 2019;132:104768. https://doi.org/10.1016/j.envi....
20.
Xuan Z, Zhong P, Li Z. Maternal active and passive smoking and risk of nonsyndromic orofacial clefts: A meta-analysis update. J Evid Based Dent Pract. 2019;19(1):62–72. https://doi.org/10.1016/j.jebd....
21.
Shao L, Zhang B, Pan X, et al. DNA methylation of IRF6 and risks of non-syndromic orofacial clefts. Oral Dis. 2019;25(5):1344–1351. https://doi.org/10.1111/odi.13....
22.
Pan X, Li P, Hu N, et al. Oxidative stress in the pathogenesis of non-syndromic cleft lip and palate. Front Physiol. 2021;12:729606. https://doi.org/10.3389/fphys.....
23.
Sun S, Jin P, Wang Y, et al. Maternal exposure to ambient air pollution and risk of orofacial clefts: An updated meta-analysis. Environ Pollut. 2021;289:117834. https://doi.org/10.1016/j.envp....
24.
Zhang B, Liang S, Zhao J, et al. Maternal exposure to air pollution and risk of non-syndromic orofacial clefts in China. Environ Res. 2018;164:461–467. https://doi.org/10.1016/j.envr....
25.
Deng K, Xing Z, Zhang H, et al. Parental occupational exposure to pesticides and risk of non-syndromic orofacial clefts: A meta-analysis. Environ Sci Pollut Res Int. 2022;29:29476–29487. https://doi.org/10.1007/s11356....
26.
Rappazzo KM, Warren JL, Meyer RE, et al. Maternal occupational exposure to organic solvents and specific birth defects in the National Birth Defects Prevention Study. Occup Environ Med. 2021;78(9):669–677. https://doi.org/10.1136/oemed-....
27.
Vajary M, Khaksarian M. A systematic review and meta-analysis on the association between maternal cadmium exposure and risk of congenital heart defects and orofacial clefts. Biol Trace Elem Res. 2018;186(2):345–352. https://doi.org/10.1007/s12011....
28.
Pi X, Qiao Y, Wei Y, et al. Association between heavy metal exposure and risk of cleft lip with or without cleft palate: A systematic review and meta-analysis. Chemosphere. 2020;259:127453. https://doi.org/10.1016/j.chem....
29.
Evlampidou I, Font-Ribera L, Rojas-Rueda D, et al. Trihalomethanes in drinking water and adverse birth outcomes: A systematic review and meta-analysis. Int J Environ Res Public Health. 2020;17(2):431. https://doi.org/10.3390/ijerph....
30.
Fucic A, Duca RC, Galea KS, et al. Reproductive health risks associated with occupational and environmental exposure to pesticides and other chemicals. Int J Environ Res Public Health. 2020;17(18):6576. https://doi.org/10.3390/ijerph....
31.
Weng H, Xia Z, Li M, et al. Gene-environment interaction between MTHFR polymorphisms and maternal exposure to environmental risk factors on non-syndromic cleft lip with or without cleft palate. Reprod Toxicol. 2021;102:1–8. https://doi.org/10.1016/j.repr....
32.
Kutbi H. Gene-environment interactions between MTHFR variants and maternal smoking in the etiology of non-syndromic oral clefts: A meta-analysis. Int J Pediatr Otorhinolaryngol. 2018;111:142–149. https://doi.org/10.1016/j.ijpo....
33.
Fan HC, Chen CY, Hsu YC, et al. Increased risk of incident nasopharyngeal carcinoma with exposure to air pollution. PLoS One. 2018;13(9):e0204568. https://doi.org/10.1371/journa....
34.
Liu Y, Wen Y, Zhang J, et al. Association of Ambient Air Pollution with Nasopharyngeal Carcinoma Incidence in Ten Large Chinese Cities, 2006–2013. Int J Environ Res Public Health. 2020;17(6):1824. https://doi.org/10.3390/ijerph....
35.
Gong W, Hu Y. Global burden of nasopharyngeal carcinoma attributable to occupational exposure to formaldehyde from 1990 to 2019. Front Public Health. 2023;11:1134268. https://doi.org/10.3389/fpubh.....
Przetwarzamy dane osobowe zbierane podczas odwiedzania serwisu. Realizacja funkcji pozyskiwania informacji o użytkownikach i ich zachowaniu odbywa się poprzez dobrowolnie wprowadzone w formularzach informacje oraz zapisywanie w urządzeniach końcowych plików cookies (tzw. ciasteczka). Dane, w tym pliki cookies, wykorzystywane są w celu realizacji usług, zapewnienia wygodnego korzystania ze strony oraz w celu monitorowania ruchu zgodnie z Polityką prywatności. Dane są także zbierane i przetwarzane przez narzędzie Google Analytics (więcej).
Możesz zmienić ustawienia cookies w swojej przeglądarce. Ograniczenie stosowania plików cookies w konfiguracji przeglądarki może wpłynąć na niektóre funkcjonalności dostępne na stronie.
Możesz zmienić ustawienia cookies w swojej przeglądarce. Ograniczenie stosowania plików cookies w konfiguracji przeglądarki może wpłynąć na niektóre funkcjonalności dostępne na stronie.